Donation Essentials Blog
Preventing Organ and Tissue Rejection
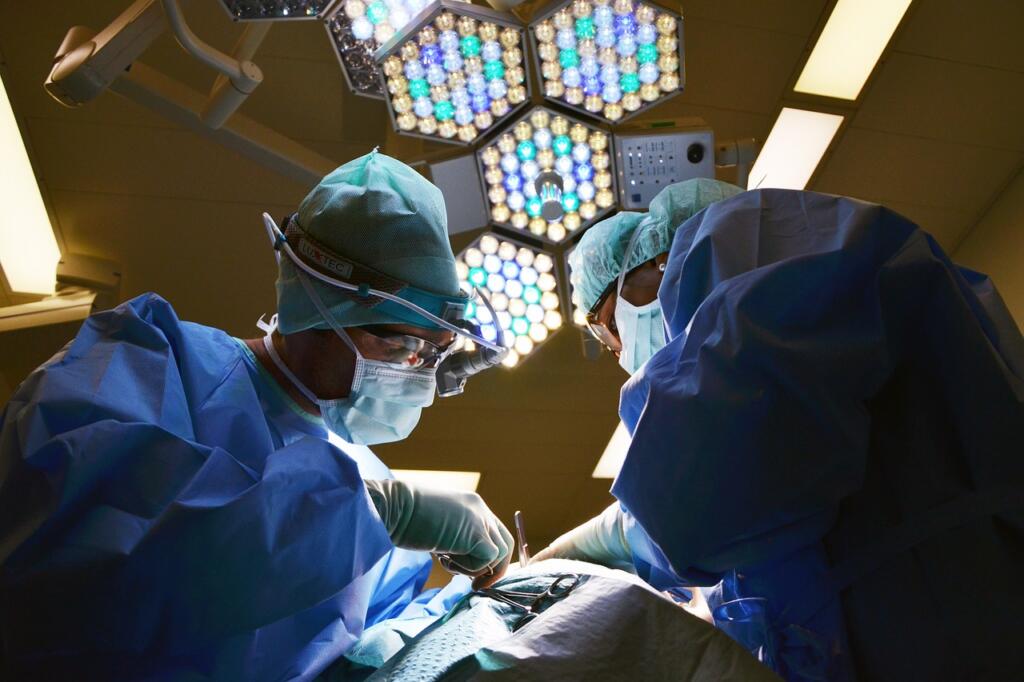
 One of the last things a patient or their family wants to worry about after they’ve received an organ or tissue transplant is whether the transplant will be rejected. But it’s important to recognize that rejection is not the same thing as losing your transplanted organ or tissue, and organ survival rates continue to improve. Read on to learn more about organ and tissue transplant rejection, rejection statistics, and how to promote organ and tissue tolerance.
One of the last things a patient or their family wants to worry about after they’ve received an organ or tissue transplant is whether the transplant will be rejected. But it’s important to recognize that rejection is not the same thing as losing your transplanted organ or tissue, and organ survival rates continue to improve. Read on to learn more about organ and tissue transplant rejection, rejection statistics, and how to promote organ and tissue tolerance.
Organ and tissue transplant rejection statistics:
Each person’s immune system reacts differently to transplanted organs, so there is no set formula to determine whether or not an organ will be rejected. However, new medications are continually being developed to reduce the risk of transplant rejection in patients. With these new medications, rejection rates are as low as 10-15 % of patients and one-year transplanted organ survival has improved to 95%. These days, rejection of tissue is uncommon.
Read more organ and tissue donation FAQs here.
Why does organ and tissue rejection occur?
Organ and tissue rejection occurs because the immune system is able to recognize transplants as foreign to the body. Normally, foreign entities are seen as threats, and in the case of viruses, bacteria, or parasites, this is a good thing! Recognizing and destroying infection quickly prevents you from developing serious symptoms.
In the case of transplants, we must trick the immune system into tolerating a foreign object in the body. It’s important to note that with every transplant, there is some level of immune system “rejection,” but in most cases, the degree of rejection will not be clinically significant. While tissue rejection is quite uncommon, there is still a low risk of rejection when it comes to organ transplants. Luckily, there are many different ways that healthcare teams and patients can decrease the risk of rejection both before and after an organ transplant.
How can you prevent organ rejection and promote immune tolerance of a transplant?
Organ rejection can be classified in one of two ways: acute rejection and chronic rejection. Acute rejection typically occurs at least within the first year after a transplant if it occurs at all. Chronic rejection occurs over a period of months or years leading to the slow loss of organ function, usually by no fault of the patient as long as anti-rejection medication is taken consistently.
To reduce the chances of transplant rejection and loss of a transplant, the following steps are taken before transplantation occurs:
- Ensure recipient and donor have compatible blood types
- Perform genetic testing to ensure compatible recipient and donor matches
- In the case of living donors, donor organs from relatives are preferred
The following steps can be taken after transplantation occurs:
- Lab results should be monitored frequently during the first year after transplant
- Anti-rejection medications should be taken consistently, at the direction of the transplant team
- A mix of different medications may be prescribed to reduce adverse side effects
- Organ recipients should also educated of the possible signs of organ rejection and alert their healthcare provider if they experience any one of the following symptoms
Interested in more organ and tissue donation facts?
Sign up for our bimonthly newsletter using the form below!
Sources: